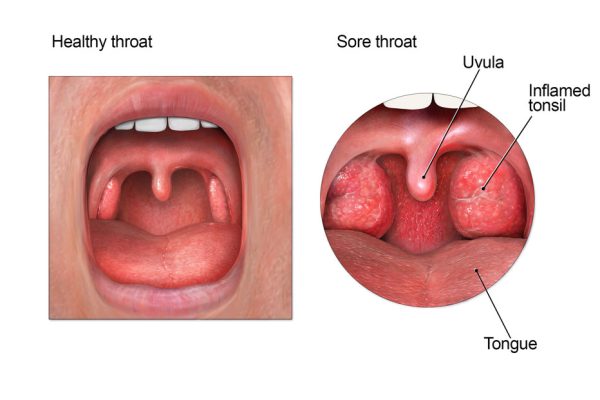
With so much happening around us, it has become hard for people to maintain a routine and follow a healthy lifestyle. The food quality and the environment around us make our bodies more prone to physical ailments. Whether it’s a headache or a surgical procedure, our body constantly looks for ways to deal with the pain. Many people rely on Percocet to control discomfort because of its easy availability as a prescription drug. These are instances where companies and government agencies run drug tests on individuals when they apply for job opportunities. Under such cases, individuals who took a dose of Percocet may fail to pass the test. An unhealthy dependency on Percocet is life-threatening and requires medical help. If this doesn’t happen, there’s little opportunity for a rebound. Read this article to learn more about Percocet and how long does Percocet stay in your system.
Table of Contents
Getting to know more about Percocet
Acetaminophen is combined with oxycodone to prepare the Percocet opioid. When these two drugs are combined, they form an effective concoction to give comfort from pain. Because of this, many people choose Percocet after medical procedures or accidents. Many individuals develop a dependency on the pain reliever which is a problem. Addiction is a result of living with long-term discomfort. Regular consumption or experimentation with a prescription drug might lead to dependence. For temporary relief of mild to extreme pain, doctors often recommend the tablet version of Percocet. The drug is excellent for individuals suffering from gastrointestinal problems and discomfort due to gallbladder stones.
You can take 2-10 milligrams of Percocet orally as your doctor prescribes. The frequency and quantity of opioid is not the same for all individuals. The dosage varies with the intensity of discomfort and pain. You must be conscious when using this pain reliever for the first time. Individuals who begin to cure their pain using Percocet tend to become dependent on the painkiller for minor pain. Eventually, they end up becoming addicted to this opioid. As time passes, the use develops into misuse. It has become a significant problem in the real world. Knowing how long does Percocet stay in your system, you can determine the right path to handle your drug misuse.
Details about how long does Percocet stay in your system
It is essential to understand how oxycodone reacts inside your system first because acetaminophen is a form of paracetamol that is safer to use. There are no particular procedures to test the presence of Percocet in the system. Panels for oxycodone and other opioids are standard in most modern drug tests. Medical professionals rarely perform paracetamol testing. The reason for this is that, unlike some other drugs, paracetamol does not have the potential to cause addiction. There is a possibility that the narcotics in Percocet could get detected in the system for about ninety days; however, the accuracy of this estimation varies between tests. Oxycodone reacts to the body and dissolves very swiftly. It immediately shows the effect by releasing its chemical compounds into your system. If you want to stay away from the addictive nature of oxycodone, It becomes imperative to understand how long Percocet stays in your system.
The majority of people who take Percocet report that its effects last for approximately six hours. People typically space their doses out over six hours so that they can remain comfortable and pain-free. Once you have understood the lingering effect of the painkiller for set it will become easy for you to prepare yourself for the upcoming drug test without consuming a large dose of the opioid. The amount of time the painkiller stays in your system is based on several factors, which we will review in the following paragraphs. Some people tend to retain Percocet for a longer time in the system because of the number of doses they take in a single dose and how chronic their pain is.
1. Urinary tract
When it comes to your urinary tract, the timeline for Percocet to remain detectable depends on how well the renal and liver systems are working. How long does Percocet stay in your system is directly proportional to the quantity of the drug and how often you take it. Urine tests frequently detect traces of Percocet use for two days after the last use of the drug. The earliest possible time for detection is a couple of hours after the initial dosage has been taken.
2. Circulatory system
There is often just a 24-hour window in which Percocet may get detected in the circulatory system. The body has a limited capacity for recognizing the levels of Percocet in the system. However, modern drug tests may pick up on the oxycodone compounds in the bloodstream along with the opioid itself. It gives a better opportunity for the detection procedure to find out the effects of Percocet. Because of this, you must have an accurate understanding of how long Percocet remains in your system.
3. Hair follicles
If you want to know how long does Percocet stay in your system of hair follicles, you must recognize that Percocet stays in your system for roughly 19 hours. Percocet is not different from other opioids when it gets tested through the hair follicles. The drug continues to affect all of your hair cells even after a significant amount of time has passed. So if you have consumed Percocet recently, there is a higher probability that the test will be positive with the hair follicle drug test. A hair test will show the presence of the substance for a month. This procedure is adequate to determine how long Percocet lasts in your system after taking a large dose or abusing it for a long time. When there is reason to suspect an individual is engaging in harmful drug use, a preferred testing method is a hair sample. However, this test is not suitable for Testing for immediate application of the pain-relieving medication.
Factors affecting how long does Percocet stay in your system
Numerous different factors have an impact on both the drug’s potency and its capacity for body storage. Once you know the prominent factors, it will be easy to find out how long does Percocet stay in your system. It will help you to maintain a healthy dose of Percocet to stay away from its dependency.
1. Your age
Young people can easily expel Percocet from their system more efficiently than older individuals. If you come under the bracket of 40 years or more, you must take extra caution when consuming an opioid. Your body will become more susceptible to harm because it will not be able to get rid of the opioid for a long time. Thus, how long does Percocet stay in your system highly depends on how old are you.
2. Duration of consumption
People often keep on consuming Percocet for an extended period without much awareness about how long does Percocet stay in your system. The drug continues to pile up in their system with prolonged use. Under such cases, it becomes easy for the tests to show up the presence of Percocet in the body. Some amount of the opioid will get trapped in the adipocytes cells of your system. It is very hard to eliminate the operate completely from your system as well as from the body fluids because of its retention in the adipose tissue
3. The efficiency of your liver
If you keep consuming Percocet for several months it put a strain on your liver function. The liver will not be able to process the entire quantity of the drug. Moreover, individuals who are any kind of ailment in their liver or kidney, tend to experience more lingering effects of consuming Percocet. Their liver function and kidneys may not perform the job of eliminating the opioid from the system efficiently and smoothly. How long does Percocet stay in your system with poor liver or kidney functioning becomes more critical.
Final words
More and more people are shifting towards the use of painkillers and other medications to get rid of the pain instantly. The number of searches for “How long does Percocet stay in your system” has increased a lot. It is not a surprise that people are curious to know more about the pain relief medication called Percocet. Your health, the amount of Percocet you took, and the duration of taking the doses, all have a role in how long the drug remains in your body. Knowing this information may help you be aware of the addiction to Percocet. You can save your life in the case of an accidental overdose. Substance misuse always leads to dependency. It’s common for individuals with a painkiller dependency to question how long the drug will be active in their system.
Arpita Das Gupta hails from the City of Taj Mahal, Agra; decided to become a full-time writer after quitting her job at a multinational organisation to pursue her dream. For the last six years, she has written on many aspects of modern life. Has a passion for writing about wellness, nutrition, culinary cultures, and everything in between. Also attended Integral University in Lucknow, where she earned a Bachelor of Technology degree in Electronics and Communications. Reading, traveling, trying out new recipes, and spending time with her kid are some of the favorite things to do.